A runner who goes too hard, too fast or too often places great mechanical stress on his body and risks exceeding his body’s ability to adapt. This is when injuries occur.
When you are injured, consulting a skilled professional not only speeds up recovery, but also helps you understand the mechanisms that are essential to prevent a repeat injury.
But who should you see? A physiotherapist? A chiropractor? A kinesiologist? An osteopath? An acupuncturist? A sports medicine doctor? The question is more complex than it sounds. Here is some advice to make a more informed choice.

Distinguishing Between Different Types of Care
There are significant variations in techniques and philosophies within and between these professions. Choosing the right professional is sometimes a daunting task for the novice. Regardless of which professional one chooses, the care provided will usually be divided into what the medical professions call active and passive modalities.
Passive modalities are the set of physical maneuvers performed directly by the therapist to accelerate and guide the injured tissue to return to normal function.
There are many passive care techniques available. Several are in fact « care systems » with protocols according to the pathologies (presentation of injury) or variants of pathologies encountered. Here are some popular names you may have heard of. The McKenzie Technique, Applied Kinesiology, Active Release Technique (ART), Graston Technique, Manual Therapy, Global Postural Rehabilitation and Subdermal Needle Therapy (also referred to as « dry needling ») are just a few of the many care techniques offered by the various physical health professionals.
I will not review the levels of evidence supporting each of these techniques in detail here. It should be noted that professionals usually require additional training or certification in order to obtain the right to practise these techniques.
Active modalities are those therapies in which the patient takes an active part in their treatment, such as muscle strengthening or relaxation exercises, education, plans for progressive return to training, and stride analysis and modification.
So for an injury, is it best to consult a physiotherapist, chiropractor or osteopath?
It is in fact impossible to offer a short and clear answer to this question, as there is a great deal of variation within each of these professions. All of the care techniques mentioned above can be used by any professional who has met the certification requirements whether they are physiotherapists, chiropractors, osteopaths, etc.
In reality, there is a vast gulf of difference between any two physiotherapists, chiropractors or osteopaths. Each professional is also free to specialize and deepen his or her knowledge in the treatment of certain conditions or a particular type of patient.
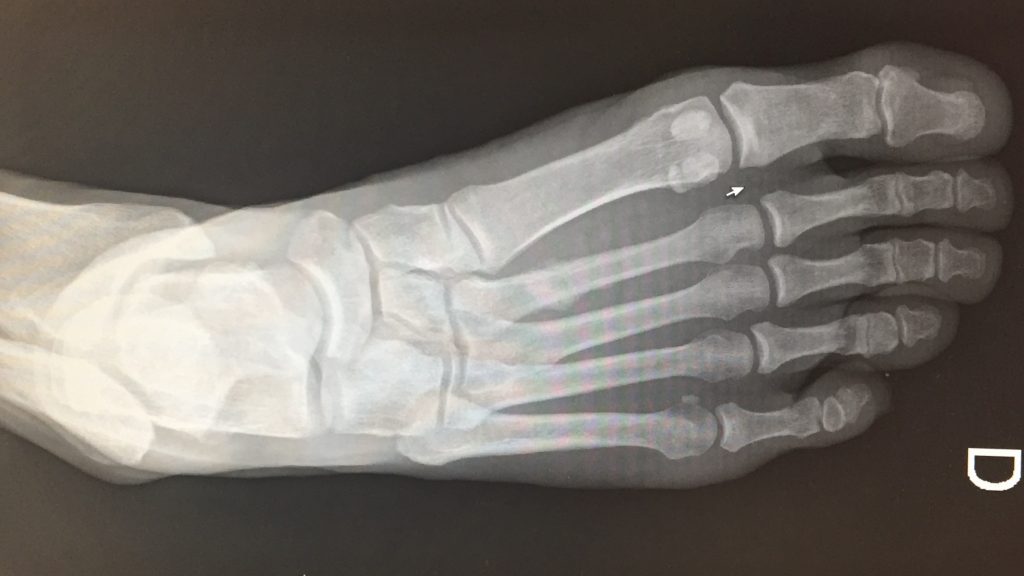
X-ray of a foot that has suffered a stress fracture to the second metatarsal.
But who is « the best?”
Once again, it is very difficult to make an objective decision about the best way to treat an injury, because a therapeutic approach usually involves a combination of several tools, each of which will be useful during the various stages of rehabilitation. This is the subjective element of these professions.
However, there are five qualities that distinguish the best therapists for treating runners:
- They must be knowledgeable, passionate about running and specialized for this particular clientele;
- They must be outstanding investigators to find the precise cause of the problem;
- They must empower the patient to take part in the process;
- They must establish a strong and trusting relationship to ensure the patient’s full adherence to their treatment plan;
- They should regularly re-evaluate the condition being treated to readjust the plan if the results are not as expected.
That being said, there are excellent therapists in each of the recognized professions. However, there is one central point regarding acute care that should be common to professionals who treat sports injuries: this is called the « quantification of mechanical stress« . There is no doubt that the best therapists, those who make a real difference, all include this essential principle in the care plans offered to their patients.
The quantification of mechanical stress is the cornerstone of any physical rehabilitation
What’s all this about? A few explanations:
The human body is made up of different bone, cartilage, tendon and muscle tissues, each of which has the potential to adapt to the mechanical stress they undergo during different activities.
Any change in the level of mechanical stress on a tissue will provoke a response. For example, if you remove all the stress induced, the tissue will atrophy and become more fragile. On the contrary, when the stress is too great and exceeds the adaptation threshold, it will cause an injury.
To use this principle as a therapeutic or preventive strategy, the professional will rigorously quantify and measure the progression of the mechanical stress levels imposed on the injured tissue. This will naturally cause the body to enact adaptation mechanisms, which will eventually make this tissue stronger, more resistant to injury and more efficient.
Let’s take the example of a stress fracture of a bone in the foot to understand the principle. This pathology is usually caused by a sudden and excessive increase in mileage, or a sudden or excessive transition to a minimalist shoe (with less cushioning in the sole).
The initial objective will be first to reduce the load on the foot as much as possible (metatarsal fractures are mostly experienced by runners), and then to reintroduce the imposed stress very gradually according to an acceptable level.
Here is a possible sequence of progression of the mechanical stress induced in the runner’s foot throughout his rehabilitation.
- Complete or almost complete reduction of loading with an Aircast boot and, sometimes, crutches, depending on pain control;
- Progressive loading with a wide shoe with a cushioned sole and little flexibility (low minimalist index), while limiting mileage according to pain threshold;
- Cross-training on a stationary bicycle with variable resistance, according to tolerance (with rigid-soled cycling shoes);
- Aquajogging, elliptical or bicycle training;
- Alternating walking/running with a Run/Walk program;
- Slowly transitioning to a shoe with a higher index of minimalism that will promote the development of stronger musculature and intrinsic bone structure of the foot to prevent relapse. As long as the stress induced respects the adaptation threshold, we remain within our « therapeutic zone,” where the body progresses towards healing. The key to success lies in the gradual progression of the intensity of the stress imposed on the injured area to move forward in rehabilitation.
The best therapists are often the most creative
The challenge is based on the ability to develop motivational cross-training (aquajogging, stationary cycling, split programs, etc.) that will allow you to continue training while controlling the amount of mechanical stress imposed on the weakened area.
So, there is no magic bullet here. Patience, perseverance and structured work will guarantee a return to a normal level of performance. You are successful when you avoid a relapse by not foolishly repeating the same mistakes through fine-tuning your training plan and running technique.
Thus, whether you consult a chiropractor, physiotherapist, kinesiologist, sports massage therapist, osteopath or doctor, the five qualities listed above are essential to seek out, and it is essential that the notion of quantifying mechanical stress be central to the suggested care plan.
Certain organizations such as The Running Clinic have a mission to offer advanced training and certification in this regard to various sports therapists. Among other things, a list of certified expert therapists can be found on their website.
Translation : William Chabot-Labbé
Must Read:
- The side effects of anti-inflammatory drugs: your need-to-know
- Is Running Ultras the Worst Idea Ever?
- Choosing a Shoe Is an Exercise in Itself: Minimalism Explained


